By Melinda Yerka
This is a painting done by Sir Charles Bell in 1809 of a soldier dying of tetanus. Doesn’t look too comfortable, hmm? Tetanus is a condition brought on when certain bacteria, called Clostridium tetani, enter deep puncture wounds, such as the proverbial rusty nail, or in this soldier’s case, a dirty sword in battle. Once inside the wound, C. tetani bacteria produce the tetanus toxin, which then migrates to the body’s central nervous system where it causes tetanus disease, characterized by intense muscle spasms. 70% to 80% of the people who contract tetanus die. Unfortunately, many of these people today are newborn infants and their mothers. Infection by C. tetani bacteria occurs in these cases when unclean instruments are used to cut umbilical cords or remove a fetus from the mother’s womb during live birth or abortion. If the mother had been immunized against tetanus toxin, she and the infant (who would be born with some of its mother’s immunities) would have survived.
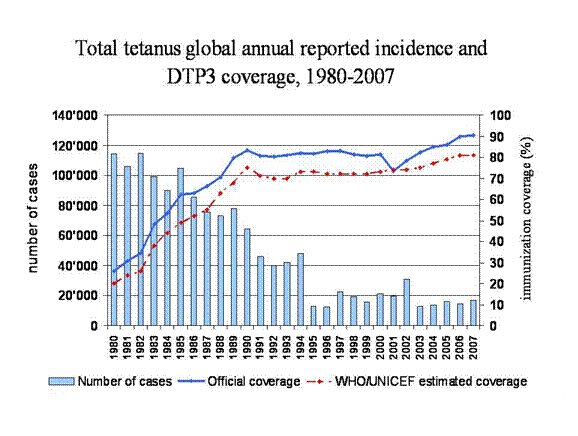
You may wonder why the mother was not immunized when vaccines against tetanus have been readily available for more than a generation. In fact, it is because vaccinations are far less prevalent in poor countries than in wealthier nations such as the United States and much of Europe. Furthermore, despite growing humanitarian interest in providing vaccines, the infrastructure of many developing nations is not sufficient to safely synthesize, transport, or store them. Lack of pharmaceutical companies, efficient transportation systems, refrigerated warehouses, and knowledgeable physicians all play a role in the continued fight against tetanus. Nevertheless, progress has been made since the early 1980’s, as depicted below in a graph from the World Health Organization (WHO).
On the left y-axis is the number of tetanus cases per year from all around the world. The blue bars represent the number of cases for each year listed on the x-axis, from 1980 to 2007. On the right y-axis is the percent of the population that has been immunized against tetanus via the DTP3 vaccine for each year. The blue line represents the percent of people who “officially” received the vaccine, and the red dotted line represents the percent of people who WHO and UNICEF estimate actually received it. Note the sharp decline in the number of tetanus cases between 1980 and 1995. This is largely due to a tremendous humanitarian undertaking by UNICEF to stamp out the disease. However, even as recently as 2007, nearly 20,000 cases per year still occur. Clearly more work remains to be done.
A novel approach to vaccination has been suggested since the mid-1990’s when genetically engineered plants began to gain rapid adoption on farms. Genetic engineering’s first really big commercial success came in the form of incorporating herbicide resistance by way of a human-created transgene into crop plants. As a result, a farmer could sow (for example) soybeans resistant to a particular herbicide, and then when weeds became a problem throughout the year, (s)he could simply spray that herbicide. All of the plants in the field except her/his soybeans would die; hence, the birth of much simplified weed control. But then came a leap of insight: why not breed vaccines into plants, too? Seeds do not require refrigeration to transport and store, nor a pharmaceutical company to produce them.
Researchers in Europe studied the possibility of incorporating a gene from C. tetani bacteria themselves, bearing resistance to the tetanus toxin, into plants. A series of feasibility studies have been conducted and their results were published by Tregoning et al. in 2005 in the European Journal of Immunology, volume 35, pp. 1320-1325. The title of their paper was “Protection against tetanus toxin using a plant-based vaccine.” In it, they report transforming the chloroplasts of tobacco plants with a gene that codes for a fragment of a protein from C. tetani that can elicit an immune response. In other words, biotechnology was used to produce a vaccine against tetanus inside tobacco plants. Tregoning et al. then immunized mice via a nasal spray (previously shown to be the most effective means of delivery) with a protein extract from transformed tobacco plants, and subsequently subjected them to a lethal dose of tetanus toxin. All mice that received the plant-based vaccine survived, while all mice that did not receive the vaccine died.
Their results are shown in the graph below.
On the y-axis is the amount of tetanus antibodies (abbreviated Anti-TetC Ig) in the mice’s blood samples. On the x-axis are the different groups of mice in the study. The Tet x1 group received the tetanus vaccine once; the Tet x2 group received it twice, the Tet x2 + CT group received it twice in addition to a cholera adjuvant designed to elicit a stronger immunity response to tetanus; finally the control group did not receive a vaccine. Where a star is above a particular group of mice’s result, it means that the average performance of that group was significantly different than the average performance of the control group. Four mice were tested in each group, and as you can see, every mouse that received the nasal spray made from the transgenic tobacco plants survived, while every mouse that didn’t died.
While it is unlikely that such transgenic tobacco plants will be grown in Africa or Southeast Asia anytime soon (no tests have yet been conducted on humans), the implications of this work are nevertheless far-reaching. They constitute the first clear proof that plants can be used to confer resistance to tetanus in mammals, and continue to push open the door that will hopefully, one day, lead to equal access to basic health care around the world.

Melinda Yerka is a graduate student studying Plant Breeding and Plant Genetics at UW-Madison. When she’s not growing weeds in the greenhouse for her research, she’s plucking weeds in her organic community garden plots.

nice post Melinda! Very informative with great graphics.
LikeLike